Methods for Administering Chemotherapy
Chemotherapy can be administered eternally (through the gastrointestinal tract) or parenterally – through some other means. When most people picture chemotherapy they picture intravenous delivery and, indeed, most cytotoxic therapy is given intravenously. But there are other methods.
Enteral methods
Most non-chemo drugs are taken orally – by pill or solution. Some chemotherapy agents are available in liquid, tablet or capsule form – the newer “targeted” therapy among them as well as hormone therapy given as an adjuvant. While patients usually prefer oral ingestion to intravenous administration, most traditional chemo agents cannot be swallowed because they would be denatured in the stomach and rendered inactive.
An advantage of oral administration is that it involves no needles (and most people find needles unpleasant). Another benefit is that patients can take the medicine at home. A disadvantage is that the medicine may irritate the digestive system. Other potential disadvantages are side effects including nausea, vomiting, diarrhea, mouth sore, hair loss and low white blood cell counts, although these side effects happen with other methods of delivery methods, too. Schedule can be once, twice, or three times a day. If you miss a dose, call the medical team. DO NOT double up dose next day. Doctors and nurses are more likely to let patients self-administer cancer drugs if they are in pill form, and some cancer patients take medicine at home. However, medical professionals worry about non-compliance and patient mistakes when medicines are taken unsupervised at home, and about drug-food interactions.
 Aside from oral, enteral methods include gastric (direct injection to the stomach) and rectal. Gastric administration can be through a nasogastric tube through the nose and down the esophagus to the stomach. The similar orogastric tube goes through the mouth. Another method of gastric administration is the percutaneous endoscopic gastrostomy tube. Rectal administration involves getting the drug into a solid form – or absorbed into or onto a solid item – and inserting the solid as a suppository.
Aside from oral, enteral methods include gastric (direct injection to the stomach) and rectal. Gastric administration can be through a nasogastric tube through the nose and down the esophagus to the stomach. The similar orogastric tube goes through the mouth. Another method of gastric administration is the percutaneous endoscopic gastrostomy tube. Rectal administration involves getting the drug into a solid form – or absorbed into or onto a solid item – and inserting the solid as a suppository.
Parenteral Methods
Paracentral administration – paracentral means any method that is not eternal but usually does not include regional application methods -is usually administration of the drug to a vein (intravenous) or an artery (intra-arterial).
Peripheral Intravenous Chemotherapy
An intravenous (IV) tube is inserted via needle into a blood vessel in the hand or arm in this method of chemotherapy. The medicine (or medicines) goes straight into the circulatory system through a vein. One advantage of this type of treatment is that the medicine enters the body quickly. Peripheral intravenous chemotherapy can also be administered in the home with the proper set-up and a visiting nurse. Disadvantages can include extravasation which is when the medicine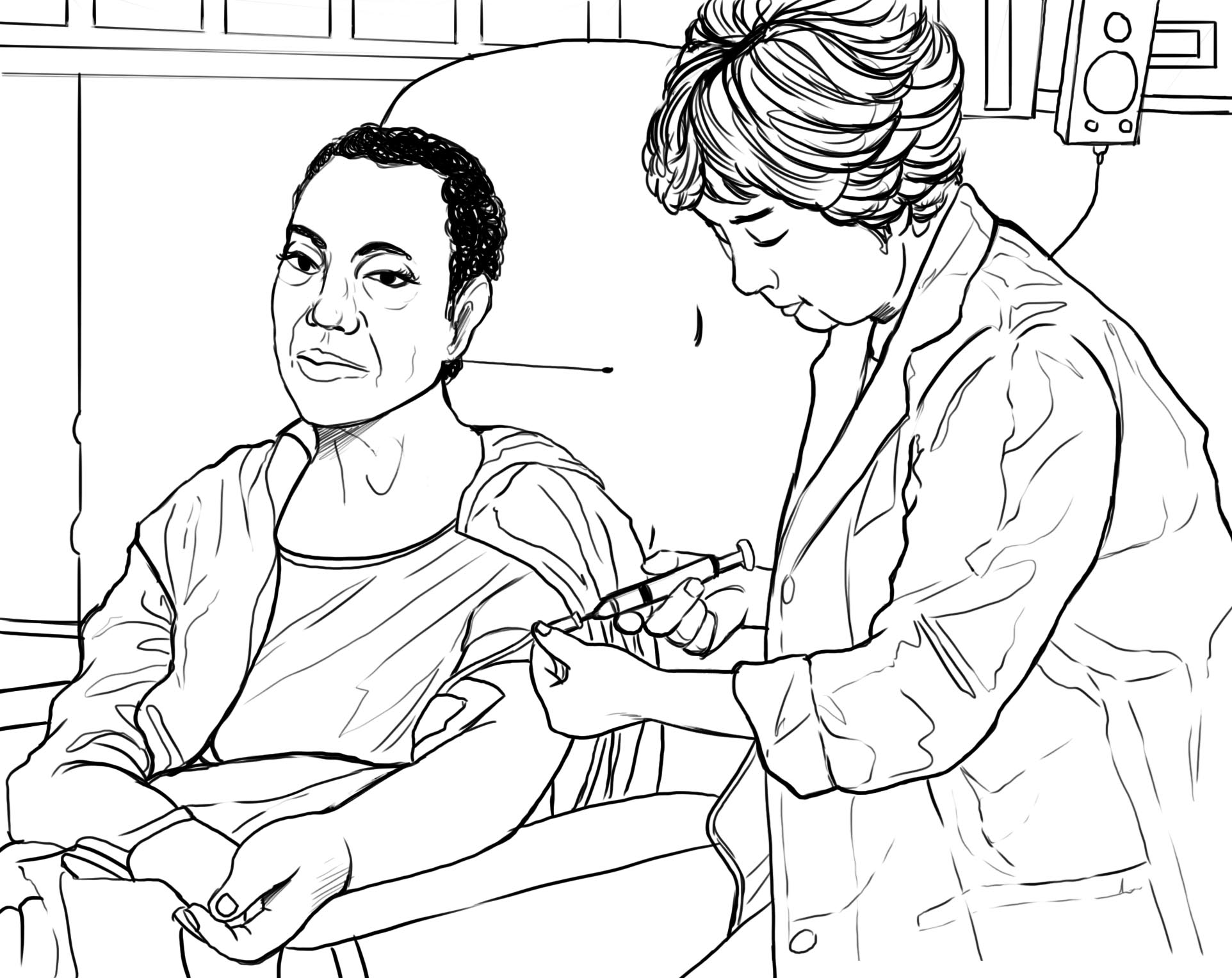 leaks out of the vein which, in turn, causes the skin to burn and blister. IV infiltration is when fluid infuses into the tissue near the entry point to the skin. It is an incorrect method of administration, but happens fairly often by accident. It is also uncomfortable to insert the needle, and the whole process is scary for some patients, at least when they start.
leaks out of the vein which, in turn, causes the skin to burn and blister. IV infiltration is when fluid infuses into the tissue near the entry point to the skin. It is an incorrect method of administration, but happens fairly often by accident. It is also uncomfortable to insert the needle, and the whole process is scary for some patients, at least when they start.
The drug is dissolved or otherwise suspended in an aqueous solution. Depending on the regimen, the drug may be injected in a matter of seconds or slowly infused over the course of hours.
The most common intravenous administration is through a temporary catheter inserted into the hand or the arm. It might take less than a minute to deliver the bolus to the patient or it might take hours – there are many regimens. A peripherally inserted central catheter is a more permanent device for patients on a course of chemo that may last up to several weeks.
Topical Chemotherapy
Anticancer drugs are applied to the skin as a lotion, cream or ointment. The advantages are that it is easy (the patient can apply medicine), quick and can be done at home. Disadvantages can include sensitive and red skin and skin that burns, discharges fluid, itches and changes color.
Intramuscular Chemotherapy
The chemotherapy is injected into a muscle in the arm, thigh or buttock. Although the shot may hurt for a bit, this is a quick way to administer chemo medicine. This type of chemotherapy can be given in the home by a healthcare professional.
Subcutaneous Chemotherapy
This type of treatment, also known as sub-q, uses a small needle that is similar to ones used by diabetics for administering insulin. Subcutaneous injections involve needle delivery of the drug under the skin but not directly into a blood vessel. An advantage to this method is that the chemotherapy medicine enters the circulatory system at a slower rate; therefore, the chances of systemic toxicity are lowered. Disadvantages can include irritation, damage to muscles, and damage to skin tissue. Intramuscular injections go deeper – though the skin – but they likewise do not enter a blood vessel directly. These delivery methods are not often used for classical chemotherapy drugs.
Intra-arterial Chemotherapy
Medicine is injected straight into an artery (through a catheter), usually to treat a single area. The catheter is placed directly into the artery that feeds the tumor. Because the chemotherapy agent is directed only to a specific area, the side effects of the drug are limited in other parts of the body. When used in brain cancer treatment, this method requires brain scans, arteriograms, anesthesia, seizure drugs and blood thinners. There is potential for hemorrhage or stroke following the procedure.
Regional Variations
Intrapleural and intraperitoneal administration involves delivering chemotherapy directly to cavities in the body that are afflicted with cancers such as mesothelioma and ovarian cancer. Hyperthermic intraperitoneal chemotherapy (Hipec), or hot chemotherapy, This technique involves application of a liquid chemotherapy agent at a temperature above body temperature (slightly over 100 degrees Fahrenheit). It is employed to treat ovarian cancer and colorectal cancer.
Intravesicular administration involves delivering medicine to the bladder via a urinary catheter. These forms of regional administration make up a minority of cases of chemotherapy.
Catheters
Today’s catheters are flexible plastic (often transparent) tubes that are employed to deliver drugs to a vein for intravenous treatment. There are many regimens for drug therapy, so the peripheral catheters may stay in for a few minutes or even up to several days.
Old catheters are not reused by other patients; they are disposed of as medical waste.
The most common site of injection is the hand or lower arm, but sometimes the point of insertion is the upper arm or neck. Central venous access devices (CVADs) are more often inserted at the neck or chest. Unlike peripheral catheters, the CVAD is closer to the central circulatory system, often being placed near a jugular vein. The catheters can be thicker in this set-up and double- and triple-lumen catheters can be employed. Lumens are the channels through the catheter. The multi-lumen catheter allows better control of pressure, parenteral nutrition, drug delivery, and taking samples of blood.
Anti-nausea medication can also be delivered by IV.
CVADs can remain in place for months. Depending on the type and stage of cancer and the medical team’s approach, some patients may need to be on chemotherapy for an extended period, and ports can make their lives easier.
Implantable ports, also called port-a-caths, are plastic or metal disks implanted beneath the skin. They offer quicker and easier access to the interior of the body for frequent application of treatment. They reduce the number of times a nurse has to prick the skin (reducing bruising) and facilitate home administration of chemotherapy. Ports can come with two or three openings for infusion of more than one medication at a time.
Port have caps which should be on them when they are not in use. Even so, there is the possibility for infection. The nursing team instructs the patient about care, including avoiding touching the port when the cap is removed, washing hands before even touching the cap, and not swimming. Blood clots are also a problem so catheters used in ports are often flushed with an anticoagulant (blood thinner) solution. Saline solution is also used to clean catheters.
Electrochemotherapy
Electrochemotherapy might sound exotic, but it’s just another way to get chemotherapy drugs into the body.
First, the patient gets chemotherapy through conventional intravenous administration or intratumor injection. Then an electrical pulse is administered somewhere on the outside of the patient’s body, probably on or near the tumor. Charging the cancer cells allows the chemotherapy agent to enter through the external membrane more easily.
The movement of the drug by this means is called electroporation. This type of administration is usually used only on skin cancers or other cancers that have spread to the skin. The chemotherapy agents are cytotoxic drugs that must enter cells to be effective, not the newer targeted agents.
Electrochemotherapy is given on an out patient basis. It is used to some extent in European countries. It is not used in the United States for humans but it is used by veterinarians on animals.
Other Forms of Chemotherapy Administration
Intralesional or Intratumoral – medicine is injected right into the tumor.
Metronomic Chemotherapy – continuous low doses. More on this.
Dose-dense Chemotherapy – a regimen in which the time between administrations of drugs is shortened. More on this.
Tattoos? – It’s still experimental, but some scientists have tried putting chemotherapy into a form that can be printed onto the skin.
Scheduling – When and how often to administer chemotherapy is a whole field unto itself.
Risk Evaluation and Mitigation Strategy
Some medicines are considered so risky that the FDA requires special monitoring of patients. The FDA has a Risk Evaluation and Mitigation Strategy (REMS) to make sure health care practitioners and patients follow administration criteria for treatments considered especially dangerous. All drugs have labels and ways they should be applied, of course, but REMS treatments are allowed only if the patient travels to a certified treatment center. Axicabtagene ciloleucel and Tisagenlecleucel are oncology drugs under REMS. The manufacturer has a website with more: https://www.yescartarems.com/ The National Cancer Institute has a page on Tisagenlecleucel here.
Related
Does it hurt? – Pain of injection is minimal most of the time. Sometimes there is a burning when the medicine courses through the blood vessels.
Locations for receiving chemo.
 Today’s arsenal of chemotherapy agents includes many different classes of medicines. Researchers continue to find and test new drugs.
Today’s arsenal of chemotherapy agents includes many different classes of medicines. Researchers continue to find and test new drugs.